How Does The Vagus Nerve Support Every Aspect Of Digestion?
Your digestive system depends upon the vagus nerve for proper function. Almost every aspect of normal digestion, motility (movement of the food/stool), and nutrient absorption depends upon proper vagus nerve function. Without the vagus nerve functioning properly, food and stool do not pass through the intestines normally.
The vagus nerve controls many aspects of optimal health! Let’s look at some organs under the control of the vagus nerve.
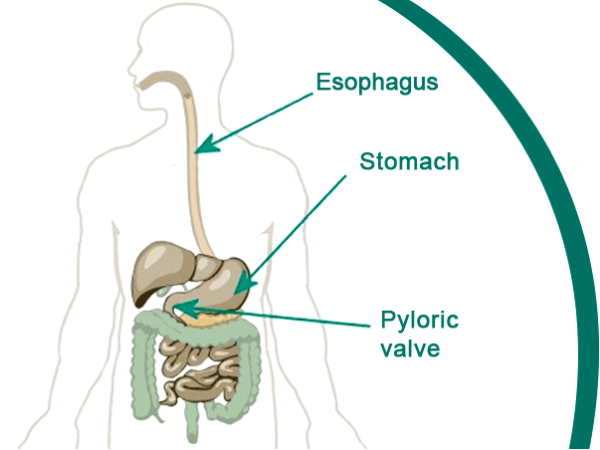
ESOPHAGUS (THROAT):
Your vagus nerve allows proper movement of food down your esophagus toward your stomach. This is called “peristalsis”.
STOMACH:
Your vagus nerve triggers your stomach to produce a healthy amount of stomach acid for proper digestion of your food, to help kill some nasty germs that can be in food, and to help with Vitamin B absorption.
PYLORIC VALVE:
The pyloric valve sits at the base of the stomach and allows food to exit the stomach and move into the intestines. The vagus nerve triggers the opening of the pyloric valve so that food does not sit in the stomach longer than necessary.
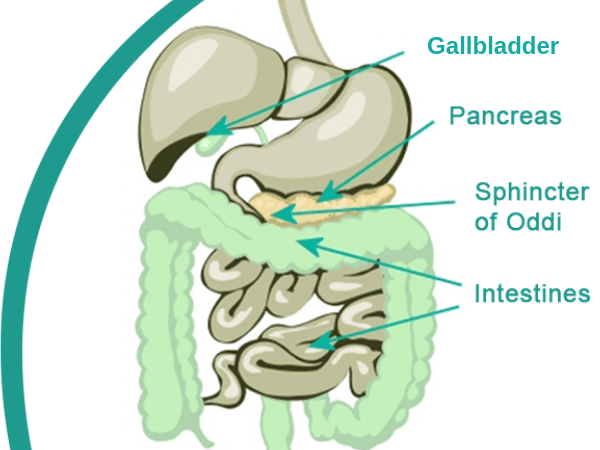
GALLBLADDER:
The gallbladder stores bile which when released, assists in the proper digestion of fats. Gallbladder function is under the control of the vagus nerve (both directly and indirectly).
PANCREAS:
The pancreas secretes pancreatic enzymes that assist in the digestion and absorption of nutrients, especially fats and proteins. The pancreas is partially controlled by the parasympathetic fibers originating in the dorsal vagal nucleus and the ambiguous nucleus of the brain, then carried by the vagus nerve.
SPHINCTER OF ODDI:
The vagus nerve stimulates the Sphincter of Oddi to open, allowing bile (from the gallbladder) and digestive enzymes (from the pancreas) to pass into the intestines.
INTESTINES:
The vagus nerve stimulates the intestines to push food (or “chime”) along the intestinal tract (“peristalsis”). Proper peristalsis mixes and shifts the chime, allowing proper nutrient absorption. Poor peristalsis can result in gastroparesis, constipation, bloating, and discomfort. If partially digested food sits in the intestines without moving, the toxins and free radicals produced are absorbed by the body. The result can be chronic inflammation of the intestinal tract, resulting in poor nutrient absorption, discomfort or pain, and constipation (often alternating with diarrhea).
INFLAMMATION:
Inflammation of the gut can contribute to poor motility (and diarrhea). The vagus nerve is critical in controlling inflammation, both through its innervation with the spleen and its direct control of many inflammatory cells. The site on the inflammatory cell under control of the vagus nerve is called the alpha-7 subunit nicotinic acetylcholine receptor (α7nAChR). As the cholinergic anti-inflammatory pathway, it is dependent upon proper vagus nerve functioning.
Parasym Plus™ is formulated to support the vagus nerve.
REFERENCES:
Ji H, Rabbi M, Labis B. Central cholinergic activation of a vagus nerve to spleen circuit alleviates experimental colitis. Mucosal Immuol. 2014 Mar :7(2):335-347 [Full Article]
Parlov VA, Tracey KJ. The vagus nerve and the inflammatory reflex – linking immunity and metabolism. Nature Reviews Endocrinology. 2012; 8:743-754. [PubMed]
Borovikova CV, Ivanova S, Zhang M, et al. Vagus nerve stimulation attenuates the systemic inflammatory response to endotoxin. Nature. 2000 May 25; 405 (6785) 458-62. [PubMed]
Mukopadhyay AK, Weisbrodt NW. Neural organization of esophageal peristalsis: role of vagus nerve. Gastroenterology. 1975 Mar; 68(3):444-7. [PubMed]
Edin R. The vagal control of the pyloric motor function: a physiological and immune histochemical study in cat and man. Acta Physio/Scand Suppl.1980; 485:1-30. [PubMed]
Qingfu L, Peng J. Sensory nerves and pancreatitis. Gland Surg. 2014 Nov; 3(4): 284-292. [PubMed]
Salvioli B. Bovara M, Barbara G, et al. Neurology and neuropathology of the pancreatic innervation. JOP.2002 Mar; 3(2):26-33. [Full Article]
Wood J, Alpers D, Andrews P. Fundamentals of neurogastroenterology. Gut. 1999 Sep; 45 (Suppl 2): 116-1116. [Full Article]
Troncom LE, Thompson DG, Ahluwalia NK, et al. Relations between upper abdominal symptoms and gastric distension abnormalities in dysmotility like functional dyspepsia after vagotomy. Gut. 1995 Jul; 37(1):17-22. [Full Article]
The NIDDAK Gastroparesis Clinical Research Consortium (6pCRC). Cholecystectomy and Clinical presentation of gastroparesis. Diq DisSci. 2013 Apr; 58(4): 1062-1073. [PubMed]
Debas H, Carvajal S. Vagal regulation of acid secretion and gastrin release. Yale Biol Med. 1994 May –Aug; 67(3-4): 145-151. [PubMed]